| .
Hazlet Office
Eatontown Office
966 Hwy 36
142 Hwy 35, Suite 106
Hazlet NJ 07730
Eatontown NJ 07724
Office
Phone:
(732) 847-3461
Office
Fax:
(732) 284-4272
Office Hours: Monday and Thursday, 8
a.m. to 5 p.m.
Venous
thromboembolism (VTE) is a frequent complication in patients who have an
acute medical illness or undergo surgery, occurring in the United States
in ~600,000 patients per year. Deep venous thrombosis (DVT) is the most
common manifestation of venous thromboembolism. This occurs when a clot
forms in the deep veins of the lower leg (calf), and can spread up to
the deep veins in the thigh. Rarely, deep veins in the upper arm can
become clotted. About 5% of all deep vein thrombosis can travel to the
lungs called a pulmonary embolism
(PE). The severity of symptoms (shortness of breath) caused by the
pulmonary emboli can be mild or in the worse situation may lead to
death.
Approximately 10% of patients die within 28 days
of developing venous thromboembolism. Pulmonary emboli account for ~10%
of in-hospital deaths, making it the most common cause of preventable
in-hospital death.
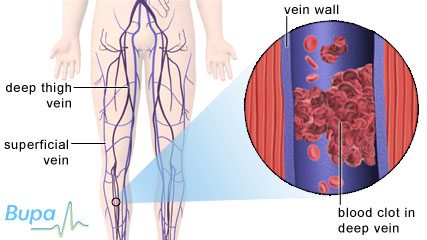
A blood clot in the deep vein of the calf which causes deep vein
thrombosis
Symptoms
Small blood clots may go undetected due to lack of
specific symptoms. Larger clots may block the blood flow in the vein and
cause symptoms such as:
- swelling of the affected leg - this is usually
different from the mild swelling of both ankles that many people
experience during long-haul flights for example
- pain in the affected leg - the pain may only be
noticeable, or get worse when standing or walking
- reddening of the affected leg
Complications
1. Pulmonary embolism
This is the most serious complication of deep
vein thrombosis. A pulmonary embolism (PE) happens when a piece of the
blood clot from a deep vein thrombosis off and travels through the
bloodstream to the lungs. In the lungs it can block a pulmonary
artery. This can cause chest pain, shortness of breath or coughing up
phlegm tinged with blood. In severe cases it can be fatal. Pulmonary
emboli happen hours or even days after the deep vein thrombosis has
formed, and may occur when there have been no obvious signs of a deep
vein thrombosis. You should seek emergency medical treatment if you
have symptoms of Pulmonary emboli.
2. Post-thrombotic syndrome
Damage to valves in the leg from a deep vein
thrombosis can eventually lead to long-term pain, swelling and,
in severe cases, ulcers on the leg.
3. Limb ischaemia
This is a rare complication that only happens in
severe deep vein thrombosis. Because of the blood clot in the leg
vein, the pressure in the vein can become very high. This can obstruct
the blood flow through the arteries, so less oxygen is carried to the
affected leg.
Causes
You are more likely to get DVT if you are over 40,
are very tall and/or if you are . If you are immobile, for example after
having an operation or , you also have a greater risk of getting DVT.
There are a number of other risk factors that make
you more likely to have DVT - these include if you have:
- had a blood clot in a vein before
- a family history of blood clots in veins
- an inherited condition that makes your blood
more likely to clot (this is called thrombophilia)
- certain blood diseases
- cancer, or have had cancer treatment
- circulation problems or heart failure
- had recent surgery or an injury, especially to
your hips or knees
- travelling on a long-haul flight (flight
lasting four hours or more)
- obese
- increased in women who:
- take a contraceptive pill that contains
estrogen
- take hormone replacement therapy (HRT)
- are pregnant
- have recently had a baby
Diagnosis
Multiple things aid in diagnosing deep venous
thrombosis:
- A good history and physical
- blood test for D-Dimer - if this is negative
it's unlikely that you have a deep vein thrombosis
- doppler ultrasound - this is the best test to
detect blood clots above the knee
- venogram - a special dye is injected into a
vein and an X-ray is then taken; this is the best way of showing
clots below the knee
Treatment
1. Medicines
Anticoagulant medicines such as heparin and
warfarin are the most common treatments for deep vein thrombosis. They
alter chemicals in your blood to stop clots forming so easily. There
are several precautions if you are taking anticoagulant medicines.
- You shouldn't take warfarin if you are
pregnant, as this will harm your baby. Your doctor can advise you
on the best treatment for you.
- You should always remind any doctor that you
are taking warfarin, especially if he or she is prescribing a new
medicine for you to take, or planning an operation.
- You shouldn't eat or drink cranberry products
while taking warfarin, as these may interfere with the way this
medicine works.
- You shouldn't do any activities that could
increase your risk of injury (especially to your head) whilst
taking anticoagulants. This is because these medicines work by
interfering with the blood clotting process, so you are more
likely to bleed and bruise while you are taking them.
2. Thrombolytic Therapy
Thrombolytic medicine works by dissolving blood
clots. It is safest when delivered directly to the clot using catheter
driven treatment.
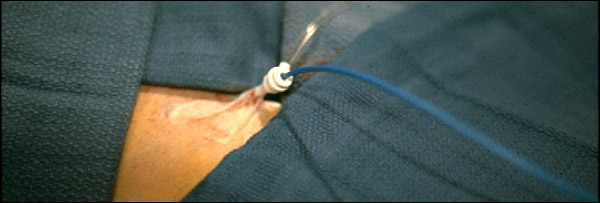 First
a devise (angio-jet system) is placed into the vein and extracts soft
clot. Then another catheter is inserted at
the area of thrombosis which drips in medicine overnight to dissolve
more chronic clot. First
a devise (angio-jet system) is placed into the vein and extracts soft
clot. Then another catheter is inserted at
the area of thrombosis which drips in medicine overnight to dissolve
more chronic clot.
This techniques is most effective immediately
after a clot forms and becomes less effective over time (after one
month). Because bleeding is a potential consequence of this treatment,
patients are usually closely monitored in the intensive care unit
during the treatment.
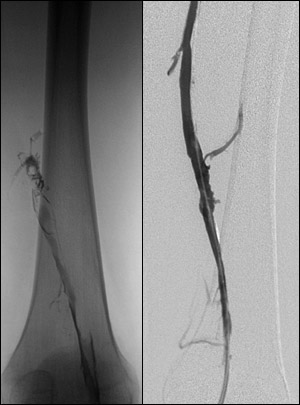
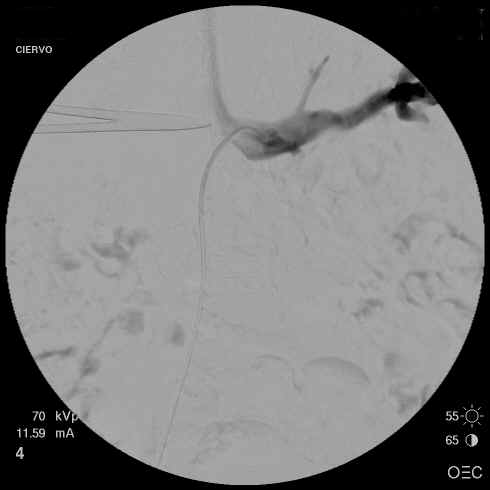
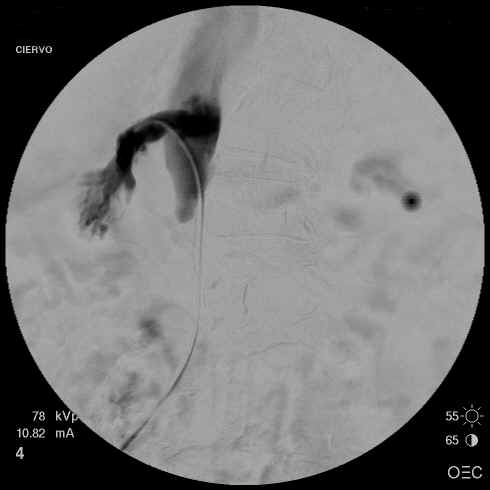
The following day, a picture of the vein is
taken (called a venogram) to see the effectiveness of the treatment.
This illustration is an example of the vein that is clotted and the
subsequent follow-up examination after treatment was given.
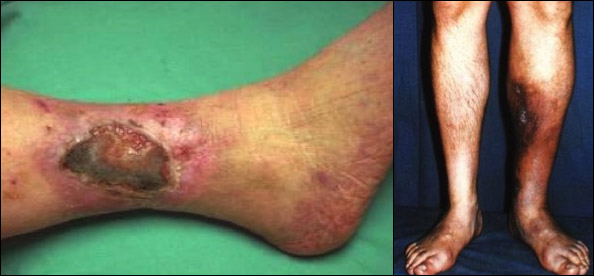
Unfortunately, some patients with
extensive clots who are unable to receive this treatmentt may develop
a condition known as chronic post-phlebitic syndrome.
Chronic swelling, discoloration of the skin and even the development
of sores may occur. If extensive clots are allowed to permanently
damage the leg veins, they cannot be dissolved later, since they
rapidly harden into scar tissue.
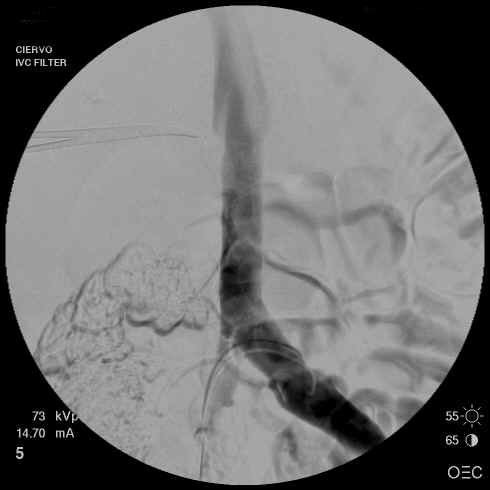
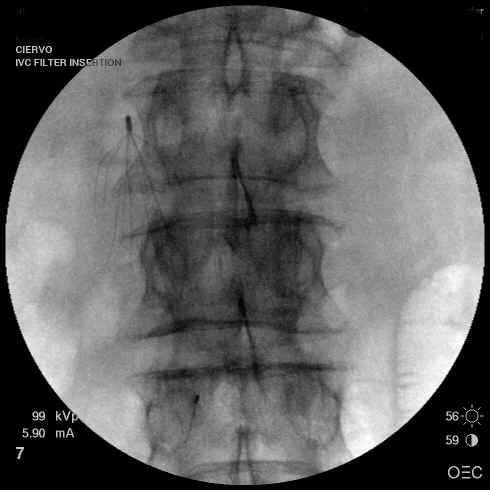
3. Inferior Vena Cava Filter Placement
This therapy is used when patients cannot
receive anticoagulant therapy. In patients with severe respiratory
compromise from the pulmonary emboli or pre-existing disease, it may
be used as a simultaneous therapeutic treatment. The procedure usually
takes less than one hour and can be done under local anesthesia in
those that are very ill.
.
4. Compression stockings
These are also known as graduated compression
stockings. Your doctor may recommend that you use these to relieve
pain and swelling, and to prevent post-thrombotic syndrome. You may
need to wear them for two or more years having a deep vein thrombosis.
Prevention
- Measures to reduce the risk of clotting include
exercising your legs regularly, for example take a brisk 30 minute
walk every day.
- An aspirin has not been proven to reduce the
risk but is routinely recommended.
- wear loose-fitting clothes
- keep hydrated by drinking enough water
- don't drink excessive alcohol or caffeinated
drinks, such as coffee
- don't take sleeping tablets, as these will stop
you keeping your legs active
- wear graduated compression stockings if you
have other risk factors for deep vein thrombosis
How can you reach us?
To
speak with a staff member, call between 9
a.m. to 5 p.m., Monday
through
Friday.
Phone:
(732)
847-3461.
|


 First
a devise (angio-jet system) is placed into the vein and extracts soft
clot. Then another catheter is inserted at
the area of thrombosis which drips in medicine overnight to dissolve
more chronic clot.
First
a devise (angio-jet system) is placed into the vein and extracts soft
clot. Then another catheter is inserted at
the area of thrombosis which drips in medicine overnight to dissolve
more chronic clot.




